[dropcap]M[/dropcap]onkeypox virus represents a double-stranded DNA virus of the genus Orthopoxvirus, genetically distinct from other viruses in this group – including variola virus (the cause of smallpox) and vaccinia virus (the virus used for the smallpox vaccine).
Human monkeypox was initially identified in the Democratic Republic of Congo (Zaire) in 1970, near the end of smallpox eradication efforts in Africa. Transmission of the disease is primarily by large droplets or direct contact, and the symptoms are similar to those of smallpox, albeit usually milder.
Monkeypox virus (MPXV) causes disease in both animals and humans. Human monkeypox, which is clinically almost identical to ordinary smallpox, occurs mostly in the rainforest of central and western Africa. The virus is maintained in nature in rodent reservoirs including squirrels.
In humans, infection with monkeypox virus results in a rash illness similar to but less infectious than smallpox. Monkeypox in humans is not usually fatal. The incubation period is about 12 days. Animal species susceptible to monkeypox virus may include non-human primates, rabbits, and some rodents.
Physicians should consider monkeypox in persons with fever, cough, headache, myalgia, rash, or lymph node enlargement within 3 weeks after contact with prairie dogs or Gambian giant rats. Veterinarians examining sick exotic animal species, especially prairie dogs and Gambian giant rats, should consider the possibility of monkeypox. Veterinarians should also be alert to the development of illness in other animal species that may have been housed with ill prairie dogs or Gambian giant rats.

Monkeypox virus is a rare zoonosis that occurs mainly in West Africa and the Congo basin.This virus and variola (smallpox) virus are the two members of the orthopoxvirus group that can produce a severe systemic illness with widespread vesiculopustular rash in humans. In its final report on smallpox eradication, the WHO considered monkeypox virus to be the most medically important orthopoxvirus in the post-smallpox era.
It has one great advantage in comparison to variola: the existence of a wide range of hosts,which would preclude worldwide eradication through a massive vaccination program. However, experiences in a recent human monkeypox outbreak showed that human-to-human transmission of this virus is quite difficult, in contrast to variola.
Some recent findings have revealed the presence of mechanisms of immune evasion that allow the virus to spread systemically and sometimes to remain dormant for long periods. These mechanisms, which may be present in variola as well, cause the induction of a state of unresponsiveness in CD4+ and CD8+ T cells when they interact with monkeypox virus–infected cells. The process seems to be MHC-independent.
The route of infection can be percutaneous, through bites or scratches of infected animals or during manipulation of infected material, or via respiratory or mucosal routes. In African endemic regions, spread of the infection is related to the hunting, skinning, preparing, and eating of infected rodents and monkeys.
The first wave of these epidemics lasted from February to August 1996 and involved 89 cases of clinical disease with six deaths. A follow-up investigation of monkeypox in the area in February 1997, which included a hut-by-hut search for active cases in 12 villages, gave evidence that up to 73% of monkeypox cases resulted from secondary human-to-human transmission.
Furthermore, three of the deaths were in children less than 3 years old and a large proportion of cases were in persons <15 years old. Thus, it appears that the outbreak is the result of the cessation of vaccination against smallpox in the late 1970s, since smallpox vaccination is also protective against monkeypox. Monkeypox virus is therefore a human pathogen that can cause fatal illness, spread from person to person, and cause outbreaks of disease in susceptible populations. To date, spread has been limited, but the potential for wider spread exits if the virus mutates so that it is more readily transmissible from person to person.
The human disease has hitherto been rare; only 400 or so cases were diagnosed in the 1980s. However, in the 1990s there were outbreaks involving more and more people. More than 500 human cases were reported in the Democratic Republic of Congo in 1996–97, the largest outbreak ever reported.
PREVENTION
There are number of measures that can be taken to prevent infection with monkeypox virus:
Avoid contact with animals that could harbor the virus (including animals that are sick or that have been found dead in areas where monkeypox occurs).
Avoid contact with any materials, such as bedding, that has been in contact with a sick animal.
Isolate infected patients from others who could be at risk for infection.
Practice good hand hygiene after contact with infected animals or humans. For example, washing your hands with soap and water or using an alcohol-based hand sanitizer.
Use personal protective equipment (PPE) when caring for patients.
SIGNS AND SYMPTOMS
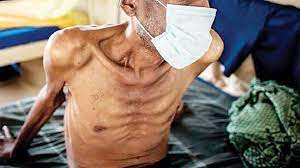
In humans, the symptoms of monkeypox are similar to but milder than the symptoms of smallpox. Monkeypox begins with fever, headache, muscle aches, and exhaustion. The main difference between symptoms of smallpox and monkeypox is that monkeypox causes lymph nodes to swell (lymphadenopathy) while smallpox does not. The incubation period (time from infection to symptoms) for monkeypox is usually 7−14 days but can range from 5−21 days.
The illness begins with:
Fever
Headache
Muscle aches
Backache
Swollen lymph nodes
Chills
Exhaustion
Within 1 to 3 days (sometimes longer) after the appearance of fever, the patient develops a rash, often beginning on the face then spreading to other parts of the body.
Lesions progress through the following stages before falling off:
Macules
Papules
Vesicles
Pustules
Scabs
The illness typically lasts for 2−4 weeks. In Africa, monkeypox has been shown to cause death in as many as 1 in 10 persons who contract the disease.
TRANSMISSION
Transmission of monkeypox virus occurs when a person comes into contact with the virus from an animal, human, or materials contaminated with the virus. The virus enters the body through broken skin (even if not visible), respiratory tract, or the mucous membranes (eyes, nose, or mouth). Animal-to-human transmission may occur by bite or scratch, bush meat preparation, direct contact with body fluids or lesion material, or indirect contact with lesion material, such as through contaminated bedding.
Human-to-human transmission is thought to occur primarily through large respiratory droplets. Respiratory droplets generally cannot travel more than a few feet, so prolonged face-to-face contact is required. Other human-to-human methods of transmission include direct contact with body fluids or lesion material, and indirect contact with lesion material, such as through contaminated clothing or linens.
The reservoir host (main disease carrier) of monkeypox is still unknown although African rodents are suspected to play a part in transmission. The virus that causes monkeypox has only been recovered (isolated) twice from an animal in nature. In the first instance (1985), the virus was recovered from an apparently ill African rodent (rope squirrel) in the Equateur Region of the Democratic Republic of Congo. In the second (2012), the virus was recovered from a dead infant mangabey found in the Tai National Park, Cote d’Ivoire.



































Leave a comment